What is mastitis?
Mastitis is a painful breast condition that occurs in breastfeeding mothers and is generally the result of a blocked milk duct that hasn’t cleared or can sometimes be caused by a knock or bump to the breast. What happens is milk within the duct gets blocked up and is eventually forced into nearby breast tissue, causing the tissue to become red, hot, painful and inflamed. The inflammation is called mastitis and although infection is generally the partner of mastitis, it is not always present in every case.
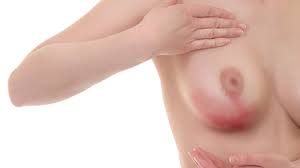
What are the symptoms of mastitis?
Early symptoms of mastitis can give you shivers and aches, a temperature and sometimes there is red welts or streaks on the affected breast. Some mothers can get mastitis quite out of the blue with no previous duct blockage or issues.
The affected breast is generally quite sore like it is with a blocked duct, only worse. It is usually swollen and hot, and red and painful to touch and move. The skin on the breast may appear shiny and striped with red streaks. You will probably feel quite ill as if you are getting a flu and it is quite common for the ill feeling to come on very quickly.
What can I do?
Firstly – please see your health care professional and then start treatment as soon as you feel a lump or sore spot in your breast.
Drain the breast often – but do so gently.
This is not the time to stop breastfeeding. More than anything else, to get rid of the mastitis your breasts need to be kept as empty as possible and your baby’s feeding at the breast is the best way to do this. Your milk is not infected in any way and it is perfectly safe for your baby to drink.
When you have mastitis, it is recommended that you feed more often than usual, starting every feed on the sore breast first and let your baby suck long enough on this side to make sure that it is being drained well.
Getting rest when you have mastitis is vital to your recover. So stayin bed if you can, or at least put your feet up for most of the day. If you can go to bed for a day or two then take your baby with you and set yourself up with nappy supplies and enough food and drinks so you don’t have to get up and down. If you have other children and can’t go to bed then setting up a daybed on the couch in the living room might suit.

There are a range of things you can do to help relieve mastitis:
- Start treatment straight away – as soon as you feel the mastitis starting or you notice a blocked duct appearing
- Rest as much as you can
- Keep the sore breast as empty as possible by feeding your baby often
- Apply warmth to the sore breast for up to a few minutes before a feed with a wheat pack or face washer that has been under hot water
- Feed from the sore breast first, when your baby’s sucking is strongest
- Massage the breast gently with your fingertips while your baby is feeding
- Change feeding positions to help shift the blockage perhaps by lying down to feed or using a football hold
- Hand express if needed, before, after and between feeds
- Cold packs after a feed may help relieve pain and reduce swelling
- Breastfeed your baby often
- Hand express if your breast feels full and your baby won’t feed often
- Early treatment will mean you get better faster, you will feel less ill and you will be at less risk of a breast abscess.
Tips to try and prevent mastitis occuring (or reoccuring):
- Ensure your baby is attaching well to your breasts and feeding well at each feed
- Breastfeed your baby as often as your baby wants to feed
- Avoid missing or putting off feeds wherever possible
- If a breast becomes uncomfortably full, wake your baby for a feed. If your baby is not interested in feeding, you may like to express a small amount for comfort
- Avoid putting pressure on your breasts eg with tight bras, fitted clothing or with your fingers while feeding
- Rest as much as you can
- Alternate from which breast you begin each feed. This can help ensure at least one breast gets drained well at every second feed
- Avoid giving your baby any other fluids except your breastmilk, unless medically advised to do so.
